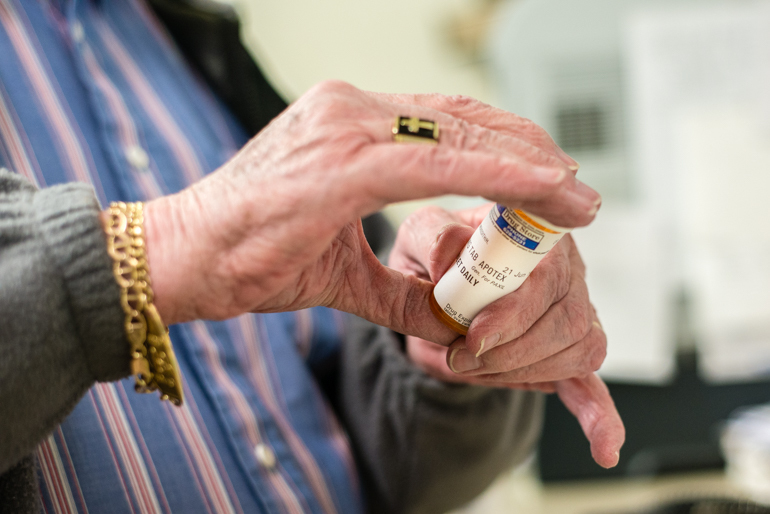
The “most important factor” that drives prescription drug prices higher in the United States than anywhere else in the world is the existence of government-protected “monopoly” rights for drug manufacturers, researchers at Harvard Medical School report today.
The researchers reviewed thousands of studies published from January 2005 through July 2016 in an attempt to simplify and explain what has caused America’s drug price crisis and how to solve it. They found that the problem has deep and complicated roots and published their findings in JAMA, the journal of the American Medical Association. The study was funded by the Laura and John Arnold Foundation with additional support provided by the Engelberg Foundation.
“I continue to be impressed at what a complex and nuanced problem it is and how there are no easy solutions either,” said lead study author Dr. Aaron Kesselheim, a professor who runs the Program on Regulation, Therapeutics and Law at Harvard Medical School and Brigham and Women’s Hospital. “As I was writing, the enormity of the problem continued to shine through.”
Five key findings in the JAMA review:
1. Drug manufacturers in the U.S. set their own prices, and that’s not the norm elsewhere in the world.
Countries with national health programs have government entities that either negotiate drug prices or decide not to cover drugs whose prices they deem excessive. No similar negotiating happens in the U.S.
When a Republican-majority Congress created the Medicare drug benefit in 2003, they barred the program that now covers 40 million Americans from negotiating drug prices. Medicaid, on the other hand, must cover all drugs approved by the Food and Drug Administration, regardless of whether a cheaper, equally or more effective drug is available. And private insurers rarely negotiate prices because the third party pharmacy benefits managers that administer prescription drugs, such as Express Scripts and CVS Health, often receive payments from drug companies to shift market share in their favor, according to the study.
2. We allow “government-protected monopolies” for certain drugs, preventing generics from coming to market to reduce prices.
In an effort to promote innovation, the U.S. has a patent system that allows drug manufacturers to remain the sole manufacturer of drugs they’ve patented for 20 years or more. The FDA also gives drug manufacturers exclusivity for certain products, including those that treat people with rare diseases.
But sometimes, drug companies deploy questionable strategies to maintain their monopolies, the study says. The tactics vary, but they include slightly tweaking the nontherapeutic parts of drugs, such as pill coatings, to game the patent system and paying large “pay for delay” settlements to generics manufacturers who sue them over these patents.
And this is a serious problem, the study concludes, because drug prices decline to 55 percent of their original brand name cost once there are two generics on the market and to 33 percent of original cost with five generics.
3. The FDA takes a long time to approve generic drugs.
Application backlogs at the FDA have led to delays of three or four years before generic manufacturers can win approval to make drugs not protected by patents, the study says.
4. Sometimes, state laws and other “well-intentioned” federal policies limit generics’ abilities to keep costs down.
Pharmacists in 26 states are required by law to get patient consent before switching to a generic drug, the authors wrote. This reportedly cost Medicaid $19.8 million dollars in 2006 for just one drug: a statin called simvastatin whose brand name is Zocor. Costs ran higher because pharmacists didn’t get patient consent and Medicaid had to pay for the costlier brand name drug even though a cheaper product was available.
5. Drug prices aren’t really justified by R&D.
Although drug manufacturers often cite research and development costs when defending high prescription prices, the connection isn’t exactly true, Kesselheim and his team found, citing several studies. Most of the time, scientific research that leads to new drugs is funded by the National Institutes of Health via federal grants. If not, it’s often funded by venture capital. For example, sofosbuvir, a drug that treats hepatitis C, was acquired by Gilead after the original research occurred in academic labs.
“Arguments in defense of maintaining high drug prices to protect the strength of the drug industry misstate its vulnerability,” the authors wrote, adding that companies only spend 10 percent to 20 percent of their revenue on research and development. “The biotechnology and pharmaceutical sectors have for years been among the very best-performing sectors in the U.S. economy.”
Instead, the price tags are based on what the market will bear, they wrote
In general, fixing America’s drug price problems won’t be easy, the study authors concluded. Congressional gridlock and the power of the pharmaceutical lobby make allowing Medicare to negotiate Part D prices an unlikely possibility. And leaving that aside, policymakers must find a way to tighten rules and strengthen oversight surrounding patent protections and exclusivity without chilling innovation, Kesselheim said.
Those not involved in the study said the fact that it was published in JAMA is meaningful because the authors are able to speak directly to doctors.
“I think the most significant thing about this is not necessarily what he’s saying but who he’s saying it to,” said Kenneth Kaitin, who directs the Tufts Center for the Study of Drug Development. “In part, the concern over rising drug prices is something that physicians have been more aware of lately…They’ve still been for the most part on the sidelines of these issues.”
Kaitin said the exception has been the American Society of Clinical Oncology and the physicians at Memorial Sloan Kettering Cancer Center.
Dr. Joshua Sharfstein, the Associate Dean for Public Health Practice and Training at the Johns Hopkins Bloomberg School of Public Health, said Kesselheim’s study provides a “bird’s eye view” of how the U.S. became an outlier when it comes to drug prices, without getting lost in the weeds.
“It also illustrates that there is not a single policy that is going to address the range of challenges that our health system faces around drug pricing,” Sharfstein said.
This story was produced by Kaiser Health News, an editorially independent program of the Kaiser Family Foundation.